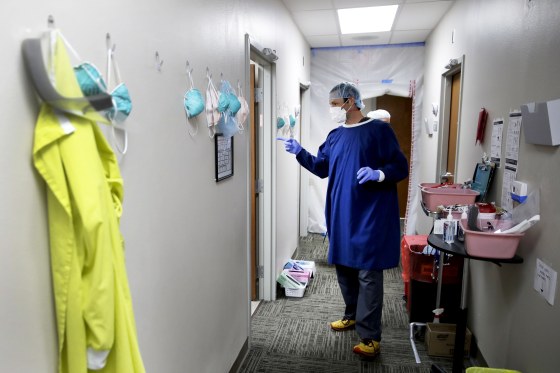
On Thursday night, Dr. Thomas Huth, vice president of medical affairs for Reid Health in Richmond, Indiana, plans to become the first person to get a coronavirus vaccine shot at his rural hospital, which will be one of the first in the country to receive the Pfizer vaccine.
His has two goals: to prevent potentially spreading the virus to his elderly patients and to communicate to the surrounding rural communities that the vaccine is safe and available.
"We plan to do that on camera in a very public way to help people feel comfortable with the vaccine," Huth said. "It's important that as a health care leader in this area, we're also leading the way on this important initiative."
Rural communities will have a particular challenge in distributing the vaccine, as officials and health care workers will have to quickly cobble together communications networks across large areas while contending with faltering and underfunded public health systems. On top of all that, distrust of medical advice is rampant — much of it shared, sown and re-emphasized by President Donald Trump, who has many supporters in rural areas.
So, beyond their work to mitigate the country's worst health disaster in modern history, health care workers in many of these regions are also having to combat bad information and encourage their patients to get the shot once it's available.

Huth said his hospital is the main point of contact for vaccinations for the four rural counties surrounding its campus in Richmond. Its officials are working to identify about 1,300 front-line health care and nursing home workers, who will be the first ones to receive the vaccine, followed by members of the general public.
The first shots — all administered to doctors — will be broadcast on a public Zoom call Thursday night, hours after the hospital first receives the vaccine, so the public can see the process and hear the doctors' thoughts. Other health care workers can begin getting vaccinated at 5:30 a.m. CT Friday.
It's important for local health care professionals to be able to say: 'Hey, I got the vaccine. It's safe, it's efficacious. I’ve looked at the data. I feel comfortable, and you should, too.'
The hospital will get only 975 doses initially, so it expects heavy competition for the vaccine, Huth said, and it is trying to figure out distribution strategies.
"The most significant communication problem is: How do you make sure we're getting all the people that we want vaccinated as soon as possible?" he said. "We want to get as many of our own staff and doctors vaccinated who are at the highest risk, and we're making efforts to set up those lists and communication networks now. But, more significantly, we want the nursing home staff to get vaccinated early, because that's where the majority of our very sickest patients come from."
'It's getting to be equivalently bad everywhere'
The vaccinations are key because the virus is hitting rural areas, like Tim Putnam's home in southeast Indiana, particularly hard. Putnam, the president and CEO of Margaret Mary Health, a community hospital in Batesville, said that the hospital has been fighting the disease since March and that "there's nothing slowing it."
It's increasingly a challenge nationwide. In the country's rural regions — where some leaders haven't required residents to follow mask mandates or other pandemic precautions — the virus is spreading at an alarming rate. The pace of transmission in those areas takes on new dimensions, as it's especially difficult to get medical care at times.
So while the vaccine feels like a godsend to many, rural providers said it would prove to be one only if they can persuade their patients to take it.
"Phase one of vaccine distribution has health care workers inoculated first, which does two things: First, I don't think anyone in the country wants to put the front-line health care staff at risk. But, almost more importantly, they're a pretty well-educated group," Putnam said. "I think acceptance in that group will help the general public in these small towns, because then they'll have someone they know who has made a pretty informed decision."
Many rural hospitals are near capacity, struggling to transfer critical patients to better-resourced medical centers and facing rampant staffing challenges.
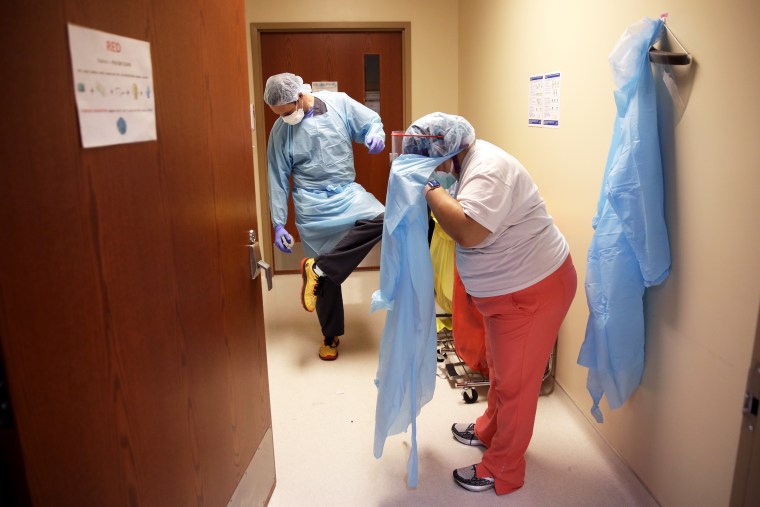
"It's getting to be equivalently bad everywhere," said Brock Slabach, senior vice president of the National Rural Health Association. "And I find that to be quite a scary condition."
Four days this month have had more deaths in America from the coronavirus than in the Japanese attacks on Pearl Harbor, Hawaii, on Dec. 7, 1941, which killed more than 2,300 people. More people in the U.S. died from Covid-19 on Wednesday than in the Sept. 11, 2001, terrorist attacks.
Perhaps in response to the steadily growing number of deaths in the United States, Americans' willingness to get the vaccine has grown in recent weeks. It has reached 63 percent, Gallup reported Tuesday, a steep climb after a low point of 50 percent in September.
While that may be an encouraging sign, the number of those vaccinated needs to be even higher for the country to return to some sense of normalcy.