Several weeks into her second pregnancy, Bianca Chavarria knew something was wrong. The baby felt strangely heavy, and there was pressure in her abdomen.
“It didn’t feel like my first pregnancy at all,” said Chavarria, then 20, of Floresville, Texas, just outside San Antonio.
Chavarria said her doctors downplayed her symptoms, so she went online to do her own research. It was then that she learned about a potentially fatal condition called placenta accreta, which occurs when the placenta won’t detach from the uterus, causing massive bleeding.

The condition, which is fatal for 7 in 100 women who develop it, tends to afflict expectant mothers like Chavarria who previously delivered children by cesarean section.
She soon learned of an additional wrinkle: Her doctor said her hospital didn’t have enough blood on hand to treat the condition. So at eight months pregnant, she was sent to San Antonio’s University Hospital, where she was quickly diagnosed with placenta accreta.
Ideally, doctors like to have months to plan for such births, but Chavarria’s baby wouldn’t wait. Two days later, in October 2021, she delivered a healthy baby boy despite experiencing massive blood loss.
“The amount of blood that we used just for Bianca’s case — a lot of hospitals don’t carry that much blood in the entire hospital,” said Dr. Caitlin Martin, who is one of the co-directors of the placenta accreta program at University Health.
The San Antonio medical center has established itself as one of the hospitals leading the way in treating placenta accreta spectrum thanks in part to its innovative blood program.

About six years ago, San Antonio launched a citywide program to make whole blood available on rescue vehicles and in its trauma centers. Numerous studies show that whole blood, which isn’t broken down into platelets and other parts after it’s collected from a donor, is the most effective treatment for people bleeding to death.
University Hospital has its own blood bank and transfusion center, which is crucial in treating a condition that results in massive blood loss.
“These cases, unfortunately, it’s almost always a question of life or death,” Martin said.
The city’s whole blood program was pioneered by a retired Air Force trauma surgeon named Donald Jenkins, who is part of a coalition of former military doctors and nurses working to make whole blood available to civilians after having seen its enormous benefits in treating soldiers on the battlefield.
“The thing that really gets me is how you can do this in a tent in the desert, and we claim we can’t do it in the cities of the United States,” Jenkins said. “That doesn’t wash.”
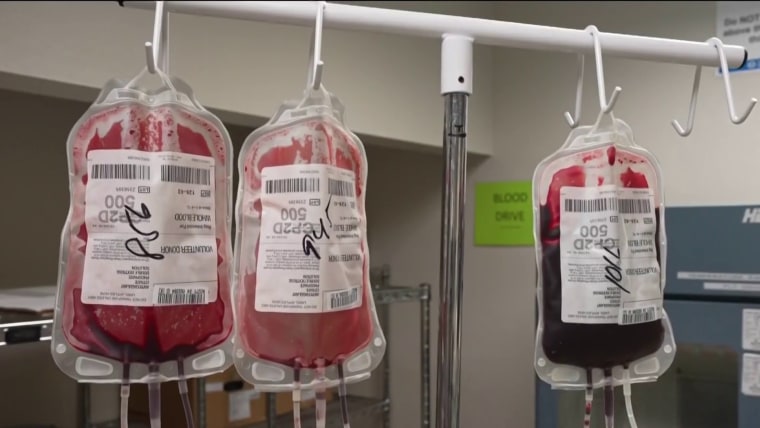
The system, which is considered a model for the country, relies on careful coordination among the local blood bank, rescue workers and the main hospital.
But the approach to treating placenta accreta patients at University Hospital goes beyond keeping a ready supply of whole blood on hand.
It employs a special unit of OB-GYNs, gynecological oncologists, trauma surgeons and other specialists who approach individual cases from every angle. They meet once a week to discuss coming placenta accreta cases and devise plans for each individual patient.
“Our team looks at the images,” Dr. Patrick Ramsey, chief of the hospital’s Maternal-Fetal Medicine division, said. “Our surgeon surgical teams are all present. Our high-risk obstetric teams are all present. Our baby doctor teams are all there. We’re all going to talk about how we’re going to coordinate that delivery to make it happen in the safest way possible.”
The focus on placenta accreta began about 10 years ago, when doctors at the hospital began to recognize that the condition was creating a life-threatening loss of blood at a much higher rate than before. About 20 years ago, it was 1 in several thousand, Ramsey said. It’s now 1 in 300 to 1 in 500 women.




